By Iris Farrou
17 Oct, 2023
Health Conditions and Pregnancy, New Moms, Parenting, Pregnancy, Prevention, Women's Health
blood pressure, early pregnancy health care, fact, genetic testing, geriatric pregnancy, Gynecologist, heart rate, high risk pregnancy, HIV, how to take care of my body when pregnant, level, Prenatal Health, prenatal visit, Rh, Screening, STD, STI, weight, when should I see a doctor after positive pregnancy test, when to see OBGYN
 Finding out you are pregnant is often very exciting, and it may come with a ton of questions as to what happens next, how you should take care of your body and your baby, how to prepare for their arrival, and all the combinations of both nervousness and excitement! Taking care of your baby begins the moment you find out you are pregnant, and seeking professional prenatal care early is key to a healthy pregnancy and successful delivery.
Finding out you are pregnant is often very exciting, and it may come with a ton of questions as to what happens next, how you should take care of your body and your baby, how to prepare for their arrival, and all the combinations of both nervousness and excitement! Taking care of your baby begins the moment you find out you are pregnant, and seeking professional prenatal care early is key to a healthy pregnancy and successful delivery.
What Do I Do?
Very good question! Most mothers have asked the same, so here is a basic checklist:
- If you suspect you are pregnant, make an appointment with your OBGYN as soon as possible. If you don’t have a regular OBGYN, call your insurance and see which experts in your area accept your insurance. If you don’t have insurance, before you look into applying, contact family planning clinics and community health centers close to you–those do provide basic prenatal care either free of charge or at a low cost.
- Your first prenatal appointment usually happens when you are 8 weeks pregnant, when a review of your medical history will take place and possibly a urine and blood test as well.
- For uncomplicated pregnancies, expect to see your prenatal healthcare provider once a month up until the 28th week, twice a month for weeks 28-36, and weekly from week 36 until delivery.
How Does this Help my Baby?
During your prenatal visits your doctor or nurse will check both your health and the health of your baby: your blood pressure and weight need to be monitored, measuring your abdomen to determine your baby’s growth is important, and your baby’s heart rate will also be checked at every visit.
Studies have shown that babies of mothers who receive no form of prenatal care whatsoever are three times more likely to have birth complications or low birth weight. It is understandable that if your insurance doesn’t cover the cost of all suggested prenatal exams and tests, you may not be able to afford them all. Some tests are screening tests, meaning that they detect risks of possible health problems; based on their results, your doctor may suggest diagnostic tests to get more accurate results.
What are some of the tests?
First and foremost your doctor needs to know your blood type and Rh factor, as well as any STIs, infections, or HIV. Genetic testing may be suggested to diagnose birth defects or possible genetic conditions, tests for chromosomal abnormalities, gestational diabetes test, glucose tolerance test, as well as regular urine tests and ultrasounds.
More
By Iris Farrou
17 Oct, 2023
Health Conditions and Pregnancy, Pregnancy, Prevention, Procedures
amnioscentesis, amniotic fluid test, fetal lung test, genetic disorders, genetic predisposition, genetic testing, gestation, Healthy pregnancy, high risk pregnancy, pregnancy health conditions, tay-sachs disease, Ultrasound
 The majority of expectant parents want to ensure their baby is as healthy as possible. Along with pre-genetic tests that determine certain genetic traits or risks parents may pass to their offspring, prenatal testings are quite common. These help you carry a healthy pregnancy to term, and check in on the baby’s health. Amniocentesis is one of these prenatal tests: it diagnoses genetic disorders and other health issues in a fetus:
The majority of expectant parents want to ensure their baby is as healthy as possible. Along with pre-genetic tests that determine certain genetic traits or risks parents may pass to their offspring, prenatal testings are quite common. These help you carry a healthy pregnancy to term, and check in on the baby’s health. Amniocentesis is one of these prenatal tests: it diagnoses genetic disorders and other health issues in a fetus:
- Fetal infection can be determined through amniocentesis, along with other illnesses
- Fetal lung testing is rarely done, but if a delivery is planned to happen sooner than 39 weeks amniotic fluid helps see if a baby’s lungs are mature enough for birth
- Sometimes there is an amniotic fluid build-up in the uterus–polyhydramnios–and it is drained through amniocentesis
What is the procedure?
It is normal to be nervous about any medical procedure, much more so if you are pregnant! The goal of amniocentesis is to extract amniotic fluid from your uterus, and most procedures happen between 15-20 weeks of gestation. Here’s what you should expect on the day of your appointment:
- You will lie on your back, just like you would prepare for a routine ultrasound. That’s the first step, as the ultrasound will show where your baby is in your uterus that particular day and time.
- The ultrasound will remain on screen as your healthcare provider inserts a very thin needle through your stomach wall and into the uterus. The needle is removed swiftly as amniotic fluid is drawn into the syringe.
- There is no sedation or numbing used, and it is important that you stay still. Even after the needle is removed, the ultrasound will remain in use to monitor your baby’s heart rate.
- You may experience mild cramping during the procedure, and/or shortly after, but you should be able to resume your normal activities after the test.
When is it necessary?
As one of many prenatal testings, amniocentesis provides details on certain genetic conditions and issues that other procedures may not fully address. It can detect chromosomal, genetic disorders, or congenital disabilities such as down syndrome, Tay-Sachs disease, neural tube defects, and Rh disease.
If the results of a routine prenatal screening test are worrisome, your doctor may suggest amniocentesis to rule out another diagnosis. If you’ve had a pregnancy with a genetic condition, amniocentesis will look for that condition in your current pregnancy. If the parents are carriers of a genetic condition, or have a family history, amniocentesis shows whether your baby is affected by it. Unusual ultrasound findings are another reason for further testing. Babies born to people over 35 have a higher risk of chromosomal conditions, so if you’ve had a prenatal cell-free DNA screening that came back positive, amniocentesis will shed light into possible conditions.
Even if your doctor suggests amniocentesis, and explains why, the final decision is up to you; as with any healthcare issue, you always have the right to seek out other professional opinions!
More
By Iris Farrou
15 Aug, 2023
Diet & Exercise, Health Conditions and Pregnancy, Heart health, Lifestyle Tips, New Moms, Parenting, Pregnancy, Prevention, Women's Health, Your baby's health
Can I use antiperspirant while pregnant, Dehydration prevention, Diet during hot summer, Dizziness, Effects of overheating on pregnancy, Exercise During Pregnancy, Fainting Prevention, high temperatures, Hot Flashes during Pregnancy, How to stay hydrated while pregnant, Overheated, Overheating while Pregnant, Pregnancy, pregnant, Protecting my baby in the heat, Regulate Body Temperature

In some parts of the country the weather is starting to cool down at this time of year, but there are still areas being affected by heatwaves. Even if you’re not in the Midwest, the South, or any other part of the US where heat persists well into September, keep in mind that bigger cities suffer higher temperatures regardless. When you’re pregnant, you have an increased amount of blood in your body, which can make you feel hotter all the time. If you combine that with the summer heat, things can get really uncomfortable…
It’s a good idea to always be aware of the risks that come with a summer pregnancy:
- You are more likely to become overheated, and suffer from dizziness, nausea, headaches, or even muscle cramps.
- With that being said, keep in mind that the chances of fainting, or losing your step and falling, are higher: this could result in a more serious injury and endanger your baby’s health–even bringing on early labor or placental abruption.
- Dehydration is one of the risks associated with overheating. If your temperature is consistently above 101 degrees, you should be seeing your doctor. High fever– especially in the first trimester–has been shown to impact fetal development, particularly the fetal heart structure and neural tube defects.
- If you work outdoors, if your job requires manual labor, if you are working in a building that’s not climate controlled, or if you work in a commercial kitchen, you should know you are at higher risk of overheating while pregnant.
Though being pregnant is not the same experience for everyone, and not all people have the same advantages, opportunities, and support from family and friends during their term, the following steps are recommended so as to keep you and your baby safe:
- Since you are liable to overheat when pregnant, try to stay out of the heat as much as possible–especially if the outside temperature is higher than 90 degrees.
- Know that if your body temperature is higher than 102 degrees for more than 10 minutes, that puts you at a higher risk for heatstroke.
- Swelling and pregnancy go hand in hand, and in the summer heat this may get worse. Try to elevate your feet as much as you can, and stretch often. If you can, avoid standing for long periods of time.
- Your body is working for two, so with a higher blood volume, you will be sweating more. That’s your body trying to keep you cool: drink lots of water to avoid dehydration, and try to wear clothes that allow heat to escape.
- Underarm antiperspirant is not your friend: you need to allow your body to regulate its temperature, so you don’t want to trap heat in you. Try to wear light, breathable fabrics that help you cool down, and always use sunscreen to protect your skin from overheating.
- If you are exercising, it is best to stay inside and use AC– it is the best thing you can do for your safety to be in climate controlled environments, drink as much water as possible, and cool down every chance you get.
- Avoid the sun, avoid high sodium foods, and avoid all other drinks but water: non-alcoholic cocktails or other drinks have sugar and other ingredients that are not helping your cause. Water should be your beverage of choice.
Always trust your instincts when it comes to how you are feeling, and always listen to your body: even if the environment is seemingly cool and safe, if you feel that something is not right, follow your gut and seek medical attention.
https://www.heart.org/en/news/2019/07/01/summer-heat-brings-special-health-risks-for-pregnant-women
https://www.cdc.gov/niosh/topics/repro/heat.html
https://www.unitypoint.org/news-and-articles/10-things-no-one-expects-during-a-summer-pregnancy
More
By Iris Farrou
31 Jul, 2023
Da Vinci Robotic Surgery, Health Conditions and Pregnancy, Hysterectomy, Menopause, Peri-Menopause, Peri-Menopause, Procedures, Queer Health, Reproductive health, Robot Hysterectomy, WNY Ob-Gyn News, Women's Health
3D imaging, abnormal vaginal bleeding, Cancer Treatment, cervical, cervix, endometriosis, faster recovery, fibroids, Laparoscopic Surgery, minimally invasive surgery, Ovarian, ovaries, pelvic pain, Precancer, Robot Assisted Hysterectomy, Robot Hysterectomy, uterine, uterine prolapse, uterus
 What is it?
What is it?
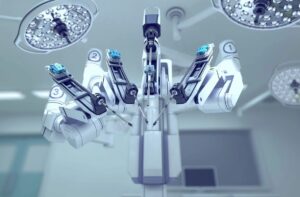
You may have heard of a traditional hysterectomy, which refers to the surgical procedure to remove the uterus (hysteros) from the body. In this case, the procedure is done with a large incision and requires longer recovery time. Nowadays, doctors can use robotic technology to their advantage–and to the advantage of the patients–to perform certain procedures, hysterectomy being one of them. In robotic hysterectomy, your doctor uses the technology to make small incisions of 1-2cm and fully controls the robotic arms with a controller while looking at a 3D magnified image of the area of surgery on their screen.
How does it work?
Robotic hysterectomy is a type of laparoscopic surgery: it is less invasive than traditional surgery, and patients experience much less pain, faster recovery, and less blood loss than open abdominal hysterectomy. Your doctor makes small incisions on your abdomen, and then inserts a laparoscope and other surgical instruments through the incisions. The laparoscope is a very thin tube with light and a camera at the end, thus projecting the surgery on a high-definition and magnified screen; this allows your surgeon to be aware of a lot more details during the surgery, as well as possible problems, than the human eye itself since the image is magnified up to 15 times.
The instruments used during robotic hysterectomy, particularly the technology of the daVinci surgical system, mimic the movement of human hands but with a lot more dexterity, precision, and flexibility. Your surgeon has full control over the instruments at all times, and they would be in the operating room just a few feet away from you. As opposed to traditional surgery where the surgeon would be standing over you for long periods of time, robotic hysterectomy allows your surgeon to utilize the constant steadiness of the robot arms to operate from angles and positions that would be typically hard to reach. Keep in mind that the robotic arms are more precise than natural hand movements, and they will not get tired during the surgery.
Who needs it?
Hysterectomies may be suggested to treat conditions like cancer or precancer of the uterus, cervix, and ovaries, uterine prolapse, endometriosis, uterine fibroids, pelvic pain, and abnormal vaginal bleeding.
Robotic hysterectomy is one of the methods surgeons can use to remove the uterus from the body, and though less invasive and more precise, surgeons decide on a case by case basis whether robotic hysterectomy is an appropriate option for their patients. Robot assisted procedures can be especially helpful if you have a complex surgical case, such as scar tissue that binds surrounding organs together and would need more precision during surgery.
What happens after it?
Like with any surgery, there will be a recovery period. Patients who have had robotic hysterectomies report that they heal faster and experience less pain; we need to remember that every body is different, and that people recover at different rates. After a robotic hysterectomy, you may be expected to stay the night at the hospital, and you may experience vaginal bleeding for a few days or weeks after your surgery. Full recovery can take 3-4 weeks, and vaginal intercourse should be avoided for at least 6 weeks after the surgery. If you are concerned about any symptoms or adverse reactions, reach out to your doctor and immediately seek professional assistance.
https://my.clevelandclinic.org/health/treatments/21057-robotic-assisted-hysterectomy
https://www.mayoclinic.org/tests-procedures/robotic-hysterectomy/about/pac-20384544
More
By Iris Farrou
16 Jun, 2023
Diet & Exercise, Health Conditions and Pregnancy, Lifestyle Tips, Nutrition, Pregnancy, Prevention, Queer Health, Women's Health
Acid Reflux During Pregnancy, Besides Tums, Digestion, Digestive Issues, Esophagus, GERD, Health Conditions while Pregnant, Heartburn, How to cure heartburn while pregnant, OTC Medication for Heartburn, Pregnancy, Pregnancy Heartburn Prevention, Preventing stomach issues, Safe Heartburn Medication, Too much calcium, What foods trigger heartburn, What stops heartburn

A large number of pregnant people experience heartburn during pregnancy, and the logical next step is to see treatment for acid reflux. There is, however, a slight difference between the two terms that may help you differentiate: acid reflux refers to the lower esophageal sphincter (LES) not tightening as it should, which allows the stomach acid to travel up to your esophagus.
Heartburn is a symptom of acid reflux, and it is often experienced as a feeling of burning or pain in your chest. During pregnancy, not only is your body changing to accommodate your baby, pushing all your gastrointestinal organs together and upwards, but your hormone levels also change and affect how you digest food.
How can it be prevented?
First things first, note that more than half of pregnant women report having heartburn in the third trimester. This is more common in women who have been pregnant before, or have experienced heartburn or dealt with acid reflux conditions before pregnancy.
Lifestyle Changes would be the first suggested method of helping you prevent heartburn during your pregnancy. One suggestion is to wear loose clothing as much as possible to avoid further constrictions on your body. You should also avoid lying down within 3 hours after a meal, and if that is not possible, make sure that your head is elevated–which can also help throughout the night as well. Additionally, lying on the left side of the body to sleep or rest has been shown to assist digestion much faster, and thus lessen the feeling of heartburn.
Eating Habits may be another element to address while pregnant. It is advised to eat smaller meals throughout the day instead of 3 big ones so that your body has more time to process the food and digest easily. Eat slowly for the same reasons, and avoid consuming fluids with your meals– instead, consume fluids in between your meals. Sitting up straight when you eat can also be of great help, as well as not eating a big meal late at night/before you sleep. Cravings may not be avoided, but do your best to pace your intake of food and respect the new–perhaps slower and more sensitive–process of your digestive system.
What are safe medications?
Most pregnant people turn to Tums as a safe medication for heartburn during pregnancy. Tums is a typical antacid with a combination of calcium, magnesium, and aluminum salts that help neutralize stomach acid. Pay attention to the dose, however, as a pregnant person should not be taking more than 1000 mg of elemental calcium per day. Additionally, when pregnant, you should avoid long term use of medications that contain magnesium trisilicate.
Your doctor may suggest other medications, specifically a medication that blocks the stomach acid from traveling up to the esophagus and contains sucralfate. A tried and true method is also to avoid citrus foods, spicy foods and caffeine, and increase how much yogurt, milk, and probiotics you take.
https://www.medicalnewstoday.com/articles/what-can-i-take-for-heartburn-while-pregnant-besides-tums#safe-medications
https://my.clevelandclinic.org/health/diseases/12011-heartburn-during-pregnancy#prevention
More
By Iris Farrou
14 Apr, 2023
Health Conditions and Pregnancy, Pregnancy, Procedures, Queer Health, Reproductive health, Surrogate, Women's Health
Buffalo NY, Cryogenic, Egg Freezing, Embryo Banking, Embryo Freezing, Fertility, Fertility Assistance, Fertility Preservation, Freezing My Eggs, How to save my eggs, Infertility treatment Buffalo, Oocyte Cryopreservation, Pregnancy and Infertility
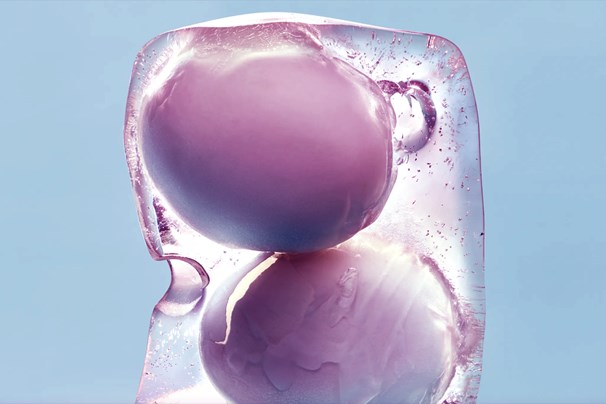
Many people consider the choice of freezing their eggs so they can retrieve them at a later time and start a family. This process is, nowadays, more common than it used to be; there is more information available for people to become aware of the pros and cons, there are more facilities that can store your eggs at an affordable price, and more professionals will suggest it if you want to have your own family later in life, or are undergoing treatments that may affect your fertility.
When Should I Consider it?
Most cis-women reach the peak of their fertility at age 30. While eggs continue to be produced and can be retrieved after that age, our egg production drops significantly around age 37, and completely stops when entering menopause–usually between 45-55 years of age. Patients who are experiencing severe health concerns that may affect their fertility– such as undergoing chemotherapy, having Polycystic Ovarian Syndrome, or endometriosis– may want to consider undergoing fertility treatments and retrieve their eggs for freezing. Egg freezing is also common among individuals who are undergoing hormone replacement therapy.
What is the Process?
It is quite a straightforward process to freeze your eggs, so don’t be alarmed by the terminologies used or the clinical equipment needed. In fact, it is very similar to the process of in-vitro fertilization, with the difference being that the eggs are not fertilized immediately, but frozen. Most cycles are complete in about 2-3 weeks.
- The first step would be to meet with a fertility specialist to discuss your desire to freeze your eggs. Then, you will schedule an exam for complete medical history, bloodwork, and hormone testing. Your doctor may also recommend a transvaginal ultrasound to assess your ovarian reserve.
- You will need to monitor your menstrual cycle and determine the exact dates when you are ovulating. To get more accurate results, your doctor may recommend birth control. After that, you will start stimulating your egg production.
- Most commonly, you will start by injecting 2-3 hormone medications a day for about ten days. This will encourage a group of eggs to develop at the same time.
- To track the ovulation and development of the eggs, you will have frequent blood work done and 4-6 pelvic ultrasounds.
- Once your eggs have matured, they will be retrieved. This involves an ultrasound-guided surgical procedure that takes 20-30 minutes under anesthesia.
And you will have reached the final step! Once an embryologist confirms the eggs are mature, which means they will have the potential to be fertilized, your eggs will head to their deep freeze home: liquid nitrogen tanks in an embryology lab.
https://www.hopkinsmedicine.org/health/wellness-and-prevention/freezing-eggs-preserving-fertility-for-the-future
https://www.healthline.com/health/egg-freezing-process#timeline
More
By Iris Farrou
07 Feb, 2023
Health Conditions and Pregnancy, Lifestyle Tips, New Moms, Nutrition, Pregnancy, Queer Health, Women's Health
Healthy weight gain pregancy, How much weight should I gain in pregnancy, How to manage weight during pregnancy, Normal weight gain during pregnancy, Pregnancy diet, Pregnancy Nutrition
 If you are expecting, or are thinking of becoming pregnant, it is possible that you are also worried about your body weight. Many expecting mothers have faced this worry before, as pregnancy significantly alters your body and is expected (and should) increase your body weight. At the same time, you want to make sure that you experience a healthy pregnancy and don’t put yourself or your baby in danger. First of all, you should remember your baby weighs around 7-8 pounds– that’s a big chunk of pregnancy weight! Additionally, your placenta, a larger uterus, and amniotic fluid add about 2 pounds each. You will also experience an increased blood volume of 3-4 pounds, and increased fluid volume of 2-3 pounds, as well as larger breasts which add 1-3 pounds. It is important to remember that your fat stores, which are much needed for a healthy pregnancy and delivery, will add 6-8 pounds.
If you are expecting, or are thinking of becoming pregnant, it is possible that you are also worried about your body weight. Many expecting mothers have faced this worry before, as pregnancy significantly alters your body and is expected (and should) increase your body weight. At the same time, you want to make sure that you experience a healthy pregnancy and don’t put yourself or your baby in danger. First of all, you should remember your baby weighs around 7-8 pounds– that’s a big chunk of pregnancy weight! Additionally, your placenta, a larger uterus, and amniotic fluid add about 2 pounds each. You will also experience an increased blood volume of 3-4 pounds, and increased fluid volume of 2-3 pounds, as well as larger breasts which add 1-3 pounds. It is important to remember that your fat stores, which are much needed for a healthy pregnancy and delivery, will add 6-8 pounds.
Though these amounts may differ from person to person, the general weight added to a mother’s body by the end of pregnancy is about 30 pounds. Most expectant mothers gain 1-5 pounds in the first trimester and 1-2 pounds per week in the second and third trimester. According to the American Pregnancy Association, a pregnant woman of relatively normal weight who gets less than half an hour of exercise every week should have a calorie intake of 1,800 in the first trimester, 2,200 in the second trimester, and 2,400 in the third trimester. It is suggested that you limit processed foods, sugars, and extra fats when you are thinking about your diet while pregnant.
The first idea that pops into mind when thinking about a healthy diet during pregnancy is supplements and vitamins. Though these are definitely important, and prenatal vitamins ensure you don’t miss out on key nutrients, you do need to decide on the specifics by consulting with your doctor or healthcare provider. It is ideal to start taking a daily prenatal vitamin at least three months before conception. Discuss your options with your doctor before deciding, as supplements need to be tailored to add on to your current diet, any special diet, health conditions, and you need to know about possible supplements that do not have a good track record and may harm your pregnancy.
Other than supplements, the principle of any healthy diet applies to pregnancy as well– make sure you consume plenty of fruits, vegetables, whole grains, healthy fats, and lean protein. Here are the nutrients that deserve special attention during your pregnancy:
- Folate and Folic Acid: this helps decrease the risk of premature birth or low birth weight. It is also a B vitamin that helps the healthy development of the brain and spinal cord.
- Calcium: you may already know calcium is necessary for healthy bones and teeth, and both you and your baby need it. Did you know that calcium also helps the circulatory, muscular, and nervous systems?
- Vitamin D: this can work together with calcium to ensure healthy bones and teeth. Vitamin D is most commonly found in fatty fish, fortified milk, and orange juice.
- Protein: you want to keep on intaking protein throughout your pregnancy as it supports your baby’s overall growth and development. You need at least 71 grams a day.
- Iron: remember that during pregnancy you need double the amount of iron that non-pregnant persons need. The body uses iron to make hemoglobin, a protein in the red blood cells that carries oxygen to the body’s tissues. If you don’t get enough iron during your pregnancy, you may be at risk of developing anemia.
https://americanpregnancy.org/healthy-pregnancy/pregnancy-health-wellness/pregnancy-weight-gain/
https://www.mayoclinic.org/healthy-lifestyle/pregnancy-week-by-week/in-depth/pregnancy-nutrition/art-20045082
More
By Iris Farrou
01 Nov, 2022
Diet & Exercise, Health Conditions and Pregnancy, Heart health, Lifestyle Tips, Mental Health, Nutrition, Pregnancy, Reproductive health, Women's Health
Anorexia and Pregnancy, Eating Disorders and Pregnancy, healthy eating, How to Eat While Pregnant, Hypertension, Mental Health Disorders During Pregnancy, Pregnancy Nutrition

The two most common types of eating disorders are anorexia nervosa and bulimia nervosa, yet there are other types out there that are not as common. Unfortunately, research on eating disorders and pregnancy is quite limited– there are estimations that eating disorders affect 5-8% of women during pregnancy, but this may not be completely credible as results can be skewed due to women’s reluctance to recognize eating disorders. Anorexia and bulimia often become noticeable in adolescence, and it’s possible that they linger during a woman’s reproductive years. Consequently, they can of course affect not only a woman’s reproductive health but also the health of her baby.
Fertility is the first affected area of women who suffer from an eating disorder: most women with anorexia do not have menstrual cycles, and approximately half of the women who have bulimia do not experience regular menstrual cycles. Absence of menstruation or irregular periods can limit the chances of conceiving, or even make it a lot more difficult for a couple to conceive. If you know you have an eating disorder and are seeking to get pregnant, it will be much healthier for you and your future baby if you try to treat your eating disorder first and establish some healthy eating habits. It is also important to share your history with medical professionals and ask for your weighing to be treated with more care.
Though there is quite a long list of complications associated with eating disorders during pregnancy, rest assured that proper planning and prenatal care– as well as a commitment to building healthy eating habits and helping your body remain healthy– can minimize a lot of those complications, lessen the risks associated with them, and enhance your chances for a healthy pregnancy. Some of those complications can be premature labor and low birth weight, as well as delayed fetal growth and respiratory problems. You may also be at a higher risk for emergency cesarean birth and other complications during labor. Gestational diabetes, preeclampsia, and even miscarriage are also possible complications. Women with eating disorders are also at a higher risk for postpartum depression, and depression during pregnancy, and are more likely to have problems with breastfeeding. Women with bulimia are at a higher risk for hypertension, and substances such as laxatives and other medications may be harmful to the development of the baby and can lead to fetal abnormalities as well.
Eating disorders unfortunately cannot be treated with medications that are pregnancy-safe. Treatment includes, first and foremost, the mother’s determination to have a healthy pregnancy and–difficult and shameful as it may be–disclosing to health professionals that you are struggling with an eating disorder. That way, your doctor will be able to tailor your prenatal visits accordingly, and know the risk factors associated with your pregnancy. The obstetrician’s care can be complemented by a registered dietitian/nutritionist and a therapist for well rounded care and medical treatment.
https://americanpregnancy.org/healthy-pregnancy/pregnancy-health-wellness/eating-disorders-and-pregnancy/
https://www.verywellmind.com/pregnancy-and-eating-disorders-4179037
More
By Iris Farrou
01 Nov, 2022
Health Conditions and Pregnancy, Lifestyle Tips, New Moms, Nutrition, Pregnancy, Women's Health, Your baby's health
Common pregnancy complications, Gestational diabetes, Gestational Diabetes Mellitus, lower diabetes risk

You may be familiar with Diabetes Type 1 and Type 2, but did you know there is also a bonus one, called Gestational Diabetes Mellitus– or Gestational Diabetes for short? Gestational Diabetes is diabetes that’s diagnosed for the first time during the gestation period, aka pregnancy. Contrary to Type 1 diabetes, GDM is not caused by a lack of insulin. Instead, it is caused by hormones produced during pregnancy that make insulin ineffective. This is also known as insulin resistance, whereby the mother’s body does not use insulin as it should. Like other types of diabetes, GDM affects how cells use sugar. About 3-8% of pregnant people in the US are diagnosed with gestational diabetes; its symptoms disappear after delivery, and the great news is that you can help control gestational diabetes!
Symptoms: gestational diabetes does not have any symptoms on its own, except increased thirst and frequent urination (which could be pregnancy related regardless). If you are risk for Type 1 diabetes because one of your parents or siblings has it, or at risk for Type 2 diabetes because you are prediabetic, over 45 y/o, may be overweight, don’t exercise often, or have previously had gestational diabetes, your doctor may deem you are at high risk for GDM and suggest you be tested.
Risks: GDM is not like Type 1 Diabetes which can cause birth defects–in fact, GDM arrives too late in a pregnancy to cause any birth defects. Insulin resistance starts showing up around Week 24. Therefore, and thankfully, the complications are manageable and preventable. Generally, gestational diabetes may cause macrosomia and hypoglycemia, which are the two major health issues associated with it. Macrosomia refers to an excessively large fetus and hypoglycemia refers to low blood sugar in the baby immediately after delivery.
Treatment: there are available treatments for gestational diabetes, and many depend on your age, overall health, and medical history. However, the most common ways to manage GDM are to regularly check your blood sugar so it stays on healthy levels, creating a healthy eating plan with your doctor and following it, being active, and monitoring your baby.
As is the case with any pregnancy complication, it is understandable that it may cause you stress. While there is no certain way to prevent stress, do know that gestational diabetes is very manageable and has very low health risks for your baby. In fact, your own stress may cause more complications during pregnancy than gestational diabetes. You can better gauge your risk for GDM by checking your family history and having a general health assessment with your doctor early on in, or even before, your pregnancy. It is advisable to attend all your prenatal appointments, voice your concerns with your doctor, and maintain a healthy lifestyle to address the possible risks of gestational diabetes.
https://www.mayoclinic.org/diseases-conditions/gestational-diabetes/symptoms-causes/syc-20355339
https://www.cdc.gov/diabetes/basics/gestational.html
https://www.hopkinsmedicine.org/health/conditions-and-diseases/diabetes/gestational-diabetes
More
By Iris Farrou
07 Sep, 2022
Diet & Exercise, Health Conditions and Pregnancy, Heart health, Lifestyle Tips, Mental Health, Parenting, Postpartum, Pregnancy, Prevention, Queer Health, Reproductive health, Women's Health
Body Changes in Pregnancy, body positive, Body Positivity During Pregnancy, Body Positivity While Pregnant, Eating Disorders and Pregnancy, Healthy Lifestyle, Healthy weight gain pregancy, How much weight should I gain in pregnancy, How to manage weight during pregnancy, how to prepare body for pregnancy, Weight Gain Support
If you have armed yourself with all the knowledge you can gather regarding the possible changes
on your body during pregnancy, then you are one step closer to dealing with the physical effect
of those changes. Some women, though they do know their body will change during pregnancy
and possibly afterwards as well, do not seem to mind it at all. Great! According to a survey of
more than 1500 women, just over 41% said they felt more negative about their bodies after
pregnancy. Which goes to show: the majority of women are struggling with body image while
pregnant. Not to mention what the body image stress is probably not helping the baby…

Is this only related to pregnancy?
Of course not… women in general are held to unrealistic expectations of beauty standards—expectations that the media and society constantly repeat. In recent years, this pressure for body perfection has worsened with the rise of social media. What is worse in pregnancy, however, is that the changes are relatively rapid, weight gain is almost always expected, feelings are exacerbated, and you may even be feeling alien in your own body. A vessel, so to speak. All of these are true: you will most likely gain weight during your pregnancy, it’s possible to develop stretch marks, and it is also a possibility that your post-partum body will not be 100% the same as your pre-pregnancy body.
This is a lot…
Yes, this can absolutely be overwhelming. Despair not! Weight gain is—and we cannot stress this enough—normal, and healthy for your baby. Also, if your doctor or nurse gives you the green light, you can exercise while pregnant. It may be light exercise, such as swimming or walking, or pre-natal yoga. These options help make you more aware of the connection between your body and your mind, perhaps take some of the edge off and your mind off of your worries and are steps to ensure the overall health of your body.
If you are concerned about weight gain during pregnancy, make a plan with your doctor, nurse, or mid wife, about your diet. Allow yourself the small pleasures without guilt: your body is participating in the miracle of nourishing a new life. There is no way to make this happen in a healthy manner unless you experience changes yourself.
What else can I do?
Honestly, don’t bottle up your feelings. Being insecure about, or even disappointed with, your
body image is completely normal. Share those feelings and thoughts with your partner, talk about
those worries with your friends. You may want to join a mom group, or even an online
discussion forum where you can exchange ideas with others on the same boat. If it gets too
much, you can always talk to a medical professional or a therapist. Even if you didn’t have body
image issues before pregnancy, it is not uncommon that future mothers start facing those worries
for the first time when they become pregnant. You are not alone in this!
More
 Finding out you are pregnant is often very exciting, and it may come with a ton of questions as to what happens next, how you should take care of your body and your baby, how to prepare for their arrival, and all the combinations of both nervousness and excitement! Taking care of your baby begins the moment you find out you are pregnant, and seeking professional prenatal care early is key to a healthy pregnancy and successful delivery.
Finding out you are pregnant is often very exciting, and it may come with a ton of questions as to what happens next, how you should take care of your body and your baby, how to prepare for their arrival, and all the combinations of both nervousness and excitement! Taking care of your baby begins the moment you find out you are pregnant, and seeking professional prenatal care early is key to a healthy pregnancy and successful delivery. 








