
When we’re getting ready to start a new family, we may find ourselves reflecting on our own childhood experiences, and comparing with our partner how each person grew up– perhaps the goal of this introspection is to create a new family that is healthy, happy, and flourishes with good communication. If you are in the process of family planning, you may want to take into account ACEs: Adverse Childhood Experiences.
What are they?
Adverse Childhood Experiences are traumatic events children experience between the ages of 0-17. These have long lasting effects, may lead to chronic health conditions, and people address them well into adulthood. It is important to remember that ACEs affect a child’s brain, and how they experience the world.
ACEs are quite common, with 60-80% of US adults reporting they have had at least one adverse childhood experience up until age 17, and 1 in 6 US adults saying they’ve had four or more. The most potentially traumatic ACEs can include experiencing violence, abuse, or neglect in the home, neighborhood, or school, witnessing violence in the community or otherwise living in a dangerous environment (war zone, poverty stricken areas, etc.), going through a natural disaster, witnessing serious injuries or the death of another person, losing a loved one or experiencing parental loss due to separation. However, this is by no means an exhaustive list of possible ACEs: any event that may cause trauma and long-term stress can be classified as an adverse childhood experience that adversely affects a person as an adult.
How do I know if my child has had an ACE?
The effects of a traumatic or stressful event may not be immediately visible, or take place soon after the traumatic event has occurred. If your child confides something in you that would be traumatic, then that is a clear indication of an event that would warrant immediate support–with the assistance of a mental health professional who specializes in children or teenagers.
Additionally, if you are going through something as a family, such as a divorce, death, fatal accident or illness, natural disaster, poverty, community violence, unemployment, housing and/or financial insecurity, you may want to address those events as potentially traumatic for your child. We cannot always correct or control life’s adversities, but we can recognize them for what they are and present this as a starting point to healing. If you recognize, as a family, that an event has been traumatic then this shows to your child that it’s ok for things to not be “normal”–that it’s part of life, and that our reactions or daily life will change when something happens.
If there is an event or experience that you do not know about, once your child has had time to process the experience you may start noticing signs of trauma that could include, but are not limited to: difficulty sleeping or having nightmares, wetting the bed, changes to their mood, fear of other people, difficulties in school, avoiding situations, events, or people (these may be directly associated with the traumatic event), as well as difficulty showing affection towards family and friends–especially if this is a change from their usual behavior.
How can we avoid ACEs?
The unfortunate truth is that we cannot completely eliminate ACEs, as much as we may want to. What we can do, however, is raise awareness about them so that we can all start thinking differently about childhood trauma. Historically disadvantaged populations are more susceptible to trauma, but that does not mean that everyone else is excluded. The causes may be societal, historical, natural forces, or people, but each one of us can help lessen the blow of an ACE: whether you are a parent, friend, caregiver, teacher, or neighbor. Raising awareness of ACEs means switching the focus from individual responsibility to community solutions: we can all help prevent ACEs, and help children develop strong coping mechanisms. It is important to reduce the stigma associated with parents who struggle to provide a safe environment for their children, and seek community and/or government support to do so. It is also important to remember that any one of us can promote safe, stable, and nurturing environments where children are present.
https://www.cdc.gov/violenceprevention/aces/fastfact.html
https://my.clevelandclinic.org/health/symptoms/24875-adverse-childhood-experiences-ace
More
By Iris Farrou
18 Aug, 2023
Childhood Health, Early Childhood Education, Fatherhood, Lifestyle Tips, Mental Health, New Moms, Parenting, Toddler Health, Young adults & teens
Abuse, Accident, ACE, Childhood Illness, Childhood Trauma, Children, Community, Divorce, Family Dynamic, Financial Stress, Grieving, Kids, Mental Health, Neglect, Nightmares, Pediatric, Pediatric Mental Health Care, PTSD, Teenager, Toddler Trauma, Trauma, Traumatic Childhood Experiences, Violence, Witness, Witnessing

In some parts of the country the weather is starting to cool down at this time of year, but there are still areas being affected by heatwaves. Even if you’re not in the Midwest, the South, or any other part of the US where heat persists well into September, keep in mind that bigger cities suffer higher temperatures regardless. When you’re pregnant, you have an increased amount of blood in your body, which can make you feel hotter all the time. If you combine that with the summer heat, things can get really uncomfortable…
It’s a good idea to always be aware of the risks that come with a summer pregnancy:
- You are more likely to become overheated, and suffer from dizziness, nausea, headaches, or even muscle cramps.
- With that being said, keep in mind that the chances of fainting, or losing your step and falling, are higher: this could result in a more serious injury and endanger your baby’s health–even bringing on early labor or placental abruption.
- Dehydration is one of the risks associated with overheating. If your temperature is consistently above 101 degrees, you should be seeing your doctor. High fever– especially in the first trimester–has been shown to impact fetal development, particularly the fetal heart structure and neural tube defects.
- If you work outdoors, if your job requires manual labor, if you are working in a building that’s not climate controlled, or if you work in a commercial kitchen, you should know you are at higher risk of overheating while pregnant.
Though being pregnant is not the same experience for everyone, and not all people have the same advantages, opportunities, and support from family and friends during their term, the following steps are recommended so as to keep you and your baby safe:
- Since you are liable to overheat when pregnant, try to stay out of the heat as much as possible–especially if the outside temperature is higher than 90 degrees.
- Know that if your body temperature is higher than 102 degrees for more than 10 minutes, that puts you at a higher risk for heatstroke.
- Swelling and pregnancy go hand in hand, and in the summer heat this may get worse. Try to elevate your feet as much as you can, and stretch often. If you can, avoid standing for long periods of time.
- Your body is working for two, so with a higher blood volume, you will be sweating more. That’s your body trying to keep you cool: drink lots of water to avoid dehydration, and try to wear clothes that allow heat to escape.
- Underarm antiperspirant is not your friend: you need to allow your body to regulate its temperature, so you don’t want to trap heat in you. Try to wear light, breathable fabrics that help you cool down, and always use sunscreen to protect your skin from overheating.
- If you are exercising, it is best to stay inside and use AC– it is the best thing you can do for your safety to be in climate controlled environments, drink as much water as possible, and cool down every chance you get.
- Avoid the sun, avoid high sodium foods, and avoid all other drinks but water: non-alcoholic cocktails or other drinks have sugar and other ingredients that are not helping your cause. Water should be your beverage of choice.
Always trust your instincts when it comes to how you are feeling, and always listen to your body: even if the environment is seemingly cool and safe, if you feel that something is not right, follow your gut and seek medical attention.
https://www.heart.org/en/news/2019/07/01/summer-heat-brings-special-health-risks-for-pregnant-women
https://www.cdc.gov/niosh/topics/repro/heat.html
https://www.unitypoint.org/news-and-articles/10-things-no-one-expects-during-a-summer-pregnancy
More
By Iris Farrou
15 Aug, 2023
Diet & Exercise, Health Conditions and Pregnancy, Heart health, Lifestyle Tips, New Moms, Parenting, Pregnancy, Prevention, Women's Health, Your baby's health
Can I use antiperspirant while pregnant, Dehydration prevention, Diet during hot summer, Dizziness, Effects of overheating on pregnancy, Exercise During Pregnancy, Fainting Prevention, high temperatures, Hot Flashes during Pregnancy, How to stay hydrated while pregnant, Overheated, Overheating while Pregnant, Pregnancy, pregnant, Protecting my baby in the heat, Regulate Body Temperature
 What is it?
What is it?
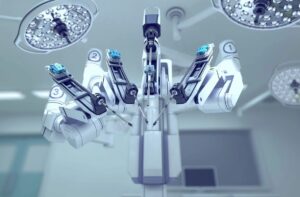
You may have heard of a traditional hysterectomy, which refers to the surgical procedure to remove the uterus (hysteros) from the body. In this case, the procedure is done with a large incision and requires longer recovery time. Nowadays, doctors can use robotic technology to their advantage–and to the advantage of the patients–to perform certain procedures, hysterectomy being one of them. In robotic hysterectomy, your doctor uses the technology to make small incisions of 1-2cm and fully controls the robotic arms with a controller while looking at a 3D magnified image of the area of surgery on their screen.
How does it work?
Robotic hysterectomy is a type of laparoscopic surgery: it is less invasive than traditional surgery, and patients experience much less pain, faster recovery, and less blood loss than open abdominal hysterectomy. Your doctor makes small incisions on your abdomen, and then inserts a laparoscope and other surgical instruments through the incisions. The laparoscope is a very thin tube with light and a camera at the end, thus projecting the surgery on a high-definition and magnified screen; this allows your surgeon to be aware of a lot more details during the surgery, as well as possible problems, than the human eye itself since the image is magnified up to 15 times.
The instruments used during robotic hysterectomy, particularly the technology of the daVinci surgical system, mimic the movement of human hands but with a lot more dexterity, precision, and flexibility. Your surgeon has full control over the instruments at all times, and they would be in the operating room just a few feet away from you. As opposed to traditional surgery where the surgeon would be standing over you for long periods of time, robotic hysterectomy allows your surgeon to utilize the constant steadiness of the robot arms to operate from angles and positions that would be typically hard to reach. Keep in mind that the robotic arms are more precise than natural hand movements, and they will not get tired during the surgery.
Who needs it?
Hysterectomies may be suggested to treat conditions like cancer or precancer of the uterus, cervix, and ovaries, uterine prolapse, endometriosis, uterine fibroids, pelvic pain, and abnormal vaginal bleeding.
Robotic hysterectomy is one of the methods surgeons can use to remove the uterus from the body, and though less invasive and more precise, surgeons decide on a case by case basis whether robotic hysterectomy is an appropriate option for their patients. Robot assisted procedures can be especially helpful if you have a complex surgical case, such as scar tissue that binds surrounding organs together and would need more precision during surgery.
What happens after it?
Like with any surgery, there will be a recovery period. Patients who have had robotic hysterectomies report that they heal faster and experience less pain; we need to remember that every body is different, and that people recover at different rates. After a robotic hysterectomy, you may be expected to stay the night at the hospital, and you may experience vaginal bleeding for a few days or weeks after your surgery. Full recovery can take 3-4 weeks, and vaginal intercourse should be avoided for at least 6 weeks after the surgery. If you are concerned about any symptoms or adverse reactions, reach out to your doctor and immediately seek professional assistance.
https://my.clevelandclinic.org/health/treatments/21057-robotic-assisted-hysterectomy
https://www.mayoclinic.org/tests-procedures/robotic-hysterectomy/about/pac-20384544
More
By Iris Farrou
31 Jul, 2023
Da Vinci Robotic Surgery, Health Conditions and Pregnancy, Hysterectomy, Menopause, Peri-Menopause, Peri-Menopause, Procedures, Queer Health, Reproductive health, Robot Hysterectomy, WNY Ob-Gyn News, Women's Health
3D imaging, abnormal vaginal bleeding, Cancer Treatment, cervical, cervix, endometriosis, faster recovery, fibroids, Laparoscopic Surgery, minimally invasive surgery, Ovarian, ovaries, pelvic pain, Precancer, Robot Assisted Hysterectomy, Robot Hysterectomy, uterine, uterine prolapse, uterus
 If you’re spending your first summer with your baby, there are a few things to keep in mind about newborn babies and the summer heat so everyone can remain safe and have an enjoyable summer. Depending on which part of the US you live in or are visiting this summer, keep in mind that the heat may continue into the fall months–or it may be humid heat rather than scorching sun. Either way, the key information to remember is that babies cannot regulate their own body temperatures– older children and adults are able to do so, but babies need extra assistance and protection.
If you’re spending your first summer with your baby, there are a few things to keep in mind about newborn babies and the summer heat so everyone can remain safe and have an enjoyable summer. Depending on which part of the US you live in or are visiting this summer, keep in mind that the heat may continue into the fall months–or it may be humid heat rather than scorching sun. Either way, the key information to remember is that babies cannot regulate their own body temperatures– older children and adults are able to do so, but babies need extra assistance and protection.
- Overheating is very risky for newborn babies: if you are hot, then your baby is definitely hot as well. It is not unusual or “wrong” to keep babies in either a light onesie or only a diaper.
- Keep the temperature cool: if you have a central AC or a window AC unit and can afford to keep it running to keep the temperature lower than 77F degrees, that is ideal for a baby. Utilizing box fans on your windows for air circulation, as well as ceiling fans, is another method to ensure your baby stays cool.
- Help them sleep comfortably: especially when sleeping, your baby can be only in a diaper or swaddled using very thin, lightweight and breathable material. If you are not using central AC, make sure there is a fan in the room where your baby is sleeping–preferably not pointed directly at them, though.
- Proper hydration: you know that’s true for people of all ages, and the same goes for babies. If you notice infrequent urination or crying without tears, these are signs that dehydration has already occurred. Your instinct may be to give your newborn baby water, but that is a big NO in this case; their bodies cannot process water. Breastfeeding or milk formula in smaller and more frequent doses are a better solution. If your baby is already eating other foods, try to use more hydrating foods in their diet and provide more frequent–but still smaller–meals.
If the outside temperature is above 90 degrees, or 84ish with humidity, this is when your newborn, toddlers, or young children should NOT be outside, especially no more than 15 minutes if you absolutely have to be out. Try to not stay in the heat for too long, and seek shelter in air-conditioned spaces.
If you are using a stroller, keep in mind that it may not be the best idea to go for a walk in the heat—however, you should choose a stroller with a large canopy for extra protection for the warmer months. Avoid going outside in peak heat times of 10am-2pm, and dress your baby in breathable cotton clothing, preferably loose, that covers their skin as much as possible. Wide hats and sunglasses do look adorable on babies, and are also very much necessary.
https://www.michiganmedicine.org/health-lab/how-protect-your-baby-dangers-hot-weather
https://www.whattoexpect.com/first-year/health-and-safety/how-to-protect-children-from-extreme-heat/
More
By Iris Farrou
27 Jul, 2023
Childhood Health, Fatherhood, Lifestyle Tips, New Moms, Parenting, Postpartum, Toddler Health, Your baby's health
are strollers too hot in the summer, Baby, Baby Safety in Summer, how do I keep my newborn safe in the sun, How to keep my baby from overheating, is central AC safe for my baby, keep my baby cool, keep my infant cool, new dads, new mom advice, new moms, newborn body temperature regulation, Toddler, toddler overheating, what clothing is best for baby in hot weather, what time of day is best to go outside during summer with newborn
 We hear the phrase “high cholesterol” many times, especially as we get older, but what does that really mean? Why are some people more prone to it than others? Cholesterol is a fat-like substance that the human body needs–in healthy amounts. Lipoproteins in our blood carry cholesterol, and when the situation gets a little out of hand high levels of bad cholesterol in our bodies cause fatty deposits in our blood vessels–this in turn can heighten the risk of a heart attack or a stroke.
We hear the phrase “high cholesterol” many times, especially as we get older, but what does that really mean? Why are some people more prone to it than others? Cholesterol is a fat-like substance that the human body needs–in healthy amounts. Lipoproteins in our blood carry cholesterol, and when the situation gets a little out of hand high levels of bad cholesterol in our bodies cause fatty deposits in our blood vessels–this in turn can heighten the risk of a heart attack or a stroke.
What to Cut Off
An unhealthy diet can contribute to developing bad cholesterol and/or the health issues that come with it; fast food, fried food, processed diets, saturated fats and trans fats are not friendly if you are trying to keep your cholesterol levels low. Saturated fats can be found in full-fat dairy products, as well as meat and butter. So, you may have to think twice about grabbing that delicious cheese tray from the store, cooking with butter, or consuming a lot of meat. Trans fats are often found in margarines and store-bought cookies and cakes–tempting, aren’t they? Not for your goal of lowering cholesterol!
Eliminating these products will help you lessen the bad cholesterol your lipoproteins carry. It’s not always easy to make diet changes, especially when your “comfort food” helps you deal with the stress of health issues, so it’s completely understandable that this situation may be a real pickle… (and no, you unfortunately should not have pickles either)
What to Add
The #1 goal when it comes to lessening cholesterol levels is to help your body absorb it into your bloodstream so as to avoid fatty deposits or clogged blood vessels. Foods with soluble fiber are particularly skilled in helping you get the “good kind” of cholesterol– oatmeal, oat bran, and high-fiber foods like fruit (eg. bananas and berries) are a great start!
Not this may sound contradictory to the discussion around “fats,” but there are good fats and bad fats. Margarine, saturated fats, and trans fats are a no-go. But, fatty acids are on your side: they can reduce triglycerides, which is another type of fat found in our blood, and help your body retain the good kind of cholesterol. Omega-3 fatty acids can be found in mackerel, herring, tuna, salmon, and trout– their fresh versions! For better results, it is recommended that you bake or grill the fish.
Almonds, walnuts, and avocados are also foods that can improve blood cholesterol and have been found to reduce the risk of heart attack. Keep in mind that nuts are high in calories so a handful goes a long way. Avocados are the good kind of fat– the opposite of saturated fat, and they are also high in nutrients and fiber. However, you can’t eat them in guacamole with dangerous chips: add plain avocado to your salads or your breakfast, or try it as a side dish.
What to Replace
Similar to fatty acids, olive oil–and especially extra virgin olive oil–can be really successful in ensuring the good type of cholesterol is absorbed by your body. You can replace pretty much any use of butter with olive oil–the difference in taste will be minimal, and the health improvements will be tremendous.
Another thing you will need to replace, and that’s not necessarily in the kitchen, is your general stance on everyday life. Lack of physical activity is a very high risk factor for heart disease–it doesn’t matter where you are on your journey or if your body can only do so much; you have to start from where you are and build up to your body’s capacity of exercising regularly. This will also slowly start to help you with maintaining a healthy weight and lessen your chances of developing heart disease, high blood pressure, or other serious health problems.
Even if you are young and healthy, and we do hope you are, remember that knowledge is always power; check your cholesterol levels during regular blood tests and doctor visits, and keep an eye on your family history for cholesterol-related diseases.
More
By Iris Farrou
21 Jul, 2023
Diet & Exercise, Heart health, Lifestyle Tips, Prevention, Women's Health
Best Foods for High Blood Pressure, Foods to Lower Cholesterol, Good Cholesterol, Healthy Diet, heart health, Heart Health Diet, How do I lower my cholesterol, LDL, Low Cholesterol Substitutes, Lower Cholesterol Foods, Meal Prep, What can't I eat with high cholesterol

Having a baby is a source of great joy for many families, single parents not excluded; it is also a big change, especially if you are an employed parent who will need accommodations to prepare for the arrival of their child. Talking to your boss or coworkers about it can be a sensitive topic, and many people may feel awkward having this conversation. First things first, it is important to know your federal rights:
- The Family and Medical Leave Act was established in 1993 to provide family and temporary medical leave under circumstances that include the birth and care of a newborn child and the placement of a child for foster care or adoption with an employee.
- Though you will need to check with your employer and meet certain provisions, the FMLA in general provides employees up to 12 weeks of unpaid leave per year. During this time, your job is protected and your health benefits should remain active.
- Upon returning to work, you also have the right to request reasonable accommodations for nursing, and other needs you may have as a new mother; the Fair Labor Standards Act protects employees from discrimination or retaliation when they assert their rights in the workspace.
With that in mind, you know you have specific laws on your side! What happens when it comes to private businesses or a work environment you’re not quite sure about? Here are some tips on how to approach your supervisors in a comfortable manner:
- Research your company’s policies on parental leave and rights; if you know you want to start a family before you start working at a specific place, that’s something you can look into early on. Knowledge is power, so you should be informed about HR processes at your workplace.
- Choose who to talk to first; if there is a chain of command, but you don’t feel comfortable approaching a certain person on it, that’s an issue HR can help you with. If you can choose who to talk to and you feel comfortable with that person, set up a meeting with them first.
- It never hurts to follow the buddy system, so consider asking a coworker you trust to be present with you in any conversations regarding parental leave and rights. Two sets of eyes and ears are better than one!
It is undeniable that you will need accommodations in the workplace during your pregnancy, before the parental leave kicks in, and that you will continue to need accommodations after you welcome your new family member.
Accommodations change throughout the duration of your pregnancy, and they differ from person to person. It is very likely that you will need different accommodations throughout your pregnancy, and of course depending on the nature of your job. Some common pregnancy accommodations may include:
- Extra breaks for restroom use, snacks, water, and rest
- Changes to job duties or location to avoid physical harm and/or fatigue
- Schedule changes and excusal from tardiness policies, as well as time for prenatal appointments
No matter the regulations or laws, it is important to remember that your health and the health of your baby and family come first; though you should feel supported by your workplace, it never hurts to know your rights and advocate for what you need.
More
By Iris Farrou
14 Jul, 2023
Fatherhood, New Moms, Parenting, Pregnancy, Queer Health
Accommodations, After Giving Birth, Corporate Policies, Coworkers, Do new fathers have time off work, Extra Bathroom Breaks, Fair Labor Standards Act, Family and Medical Leave Act, FMLA, HR, Maternity Leave, Office Job, Parental Leave, Paternity Leave, Policies, Pregnant and Working, Time Off after Birth, Will I lose my job after having a baby, Workplace

If you were a queer woman growing up in the 80s and 90s, your sex education probably consisted of mostly heteronormative standards, focusing on relationships between men and women, assuming heterosexuality as the standard overall. If you had a progressive teacher or parents, you may have been exposed to healthy examples of same-sex relationships (fingers crossed!). But, for most women who are now either well into their adult life or are parents themselves, there is a general lack on queer sex education. If like many of us, you have been fed myths, here are some that can be easily refuted:
Myth 1: Lesbian and Bisexual Women don’t get STIs
That is absolutely not the case. We may believe that the risk of Sexually Transmitted Infections between women is relatively low, but new research suggests this is not the case. In fact, lesbians are at as much risk as heterosexual women when it comes to getting an STI. Even if you are very careful in your intimate relationships and the risk is low, that does not mean that lesbians and bisexual women are not prone to STIs.
Along with dispelling this myth, we should bring up the fact that many women who identify as lesbians may have had sexual relations with men in the past–they may be carrying STIs without even knowing it. Consider this especially true for bisexual women, who may be sexually active with partners of all genders. Vaginas have the ability to fight off STIs naturally–to a certain level–while penises do not have that ability.
Face the Taboos
Many people in the queer community may identify as one gender, but carry the biological bits of another gender; if you are further exploring your own sexuality, or if you are parenting a child who is or is already a member of the queer community, it is important to keep this information in mind and not shy away from discussing matters of sexual health on all fronts. “The talk” has become more complicated, but it is our responsibility to remain educated and parent openly.
Myth 2: STIs Cannot be Transmitted Between Women
Bold lie. If you were ever told that, or have a partner/friend/family member who believes that–it is a lie. STIs are transmitted mostly through the exchange of bodily fluids, and some STIs are also contracted through skin-to-skin contact. Additionally, the risk of STI transmission is higher during menstruation.
Face the Taboos
STIs can be transmitted through oral to vaginal/vulva contact; oral-anal contact also places the participants at high risk of infections. STIs like herpes, syphilis, hepatitis A and intestinal (gut) infections, as well as possibly gonorrhea may be transmitted in this manner. Genital contact can spread HPV, pubic lice, and herpes. Fingers-in-vagina also carry the risk of transmitting herpes, HPV and bacterial vaginosis, trichomonas, chlamydia, and gonorrhea. This is especially true if one of the partners has been previously exposed to those STIs through an infected person. Use of toys that may be inserted in the vagina or anus can absolutely place the partners at risk of infection; washing the toys is not enough– you will only be 100% safe by using condoms on them.
Myth 3: Queer Women Don’t Need PAP smears
If the above two myths have shown us anything, it is that everyone is at risk of contracting an STI–no matter their sexual preferences. PAP smears are recommended for all sexually active women, even if they have never had sexual contact with a cisgender male. This is a good resource on HPV transmission : https://www.gmhc.org/resource_category/hiv-aids-information/
Myth 4: There is no Safe Lesbian Sex
Wrong! As mentioned above, the no-brainer would be to use condoms on toys (shared or not). Use different condoms for each partner, and when switching orifices. If you have any cuts or open sores on the mouth and lips, it is recommended that you use a dental dam during oral sex to protect yourself from contracting any STIs. Since some infections are transmitted by hands, always make sure that you thoroughly wash your hands before and after sex; if you have cuts or sores on your hands, you can always use a latex glove–or as many as you need!
Any member of the queer community has the right to respectful and knowledgeable treatment by their healthcare professionals. If you are having trouble finding queer-friendly health professionals, for any health issue, in your are or somewhere you are visiting, this resource can help you locate queer-safe providers: https://www.glma.org/
More
By Iris Farrou
29 Jun, 2023
Lifestyle Tips, Mental Health, Prevention, Queer Health, Reproductive health, Sexual health, Women's Health, Young adults & teens
Bisexual Sex Health, Can Lesbians get STDs?, Do I have AIDs, Do I need a PAP smear, Do Lesbians Need to See Gynecologist, gay woman, Gender Identity, Lesbian, Lesbian Sexual Health, Non-binary Health, Nonbinary, Queer Sexual Health, queer woman, Safe Lesbian Sex, Sex Health, Transgender

The first concern every parent has when it comes to their child’s health is to keep them safe as much as possible. With extracurricular activities, summer camps, and attending school being a normal part of any child’s life, and going hand in hand with exposure to germs, it is often a challenge to help your children’s immune system stay strong. There are two routes that can assist you in this struggle: diet and lifestyle.
Before we talk about details on either path, there is one undeniable basis: make sure your children are up to date on important vaccines. For all people 6 months and older, the flu shot is recommended. COVID vaccines are now safe for younger ages as well–make sure all eligible family members are immunized, and keep checking with your pediatrician about being up to date on other necessary immunizations.
Diet and Supplements
In an ideal world, you have the time to prepare the best and healthiest meals for your family, and your children are never picky eaters. That would be a wonderful movie, but it is not the truth. Though pediatricians advise against using supplements and multivitamins to enrich your child’s diet–particularly because those are not well regulated in the US and their ingredients are not guaranteed–there are certain cases when supplements are needed.
Vitamin D is the first vitamin that helps children build a strong immune system; they usually would absorb it from the sun. However, if you do not live in a sunny area, there are certain kid-friendly foods that can help with that: fortified Vitamin D milk and yogurt, and orange juice. If you are lucky enough to be able to serve your child salmon, trout, tuna, and sardines then you are raising their chances of absorbing the necessary amount of Vitamin D. To use supplements, it is suggested that you first consult with your doctor and do a blood panel to see where your child’s Vitamin D levels are at, and what supplement is most appropriate for them.
Zinc is an important mineral that assists kids’ immune system. Oysters, red meat, and poultry are the best sources of zinc, followed by beans and nuts. If your child does not accept any of these foods, consult your pediatrician on how to proceed with a zinc supplement.
Probiotics and prebiotics play an important role in our immune system, specifically because they ensure good gut health. Probiotics ensure a good balance of helpful bacteria in our bodies, and in addition to yogurts you can try giving your child fermented foods–like pickles or miso–to help with that. Prebiotics also stimulate the growth of good bacteria, and they are mostly plant fibers: green bananas or plantains, yams, asparagus.
Lifestyle
Keep in mind that a healthy lifestyle is additional to a balanced diet when it comes to fortifying your child’s immune system. If you don’t have fruits and vegetables, as well as nuts and seeds in their diet, lifestyle changes can only do so much.
However, keep in mind that children need lots of sleep for their system to function properly and recharge. 12-16 hours for infants and around 10 hours for kids is what’s necessary to assist your kids in being healthy and help keep them on a regular schedule. Additionally, exercise and keeping active can do wonders for our immune system: encourage your child to be physically active at least one hour a day in some form of activity that they like; if they appreciate sports, so much the better! Physical activity doesn’t only contribute to overall good health, but it also helps manage stress. When we are stressed, especially in cases of heightened or chronic stress, our immune system is volatile and makes us more prone to infections. Be mindful of the stress levels your child may be facing, and encourage activities that make them happy and fulfilled.
https://www.health.harvard.edu/blog/boosting-your-childs-immune-system-202110122614
https://health.clevelandclinic.org/how-to-boost-your-kids-immunity/
More
By Iris Farrou
22 Jun, 2023
Childhood Health, Diet & Exercise, Fatherhood, New Moms, Parenting, Prevention, Toddler Health, Women's Health, Young adults & teens, Your baby's health
Anxiety, Baby, Boost Immunity, Child, food, Good Health, Immune System, Immunizations, Importance of, Pre-Teen, Probiotics, Sleep, Strengthen, Stress, Toddler, Vaccine, Vaccines, Vitamins, Wellbeing

Most parents nowadays try to ensure their kids have a well rounded education when it comes to sexual health and safety, and “the talk” has been appropriately modified–in most households–to expand beyond the heteronormative model of sexual intimacy. Teenagers are exposed to diverse models of relationships, and abundant resources are available for those who explore their sexual and gender identity.
Despite the positive rise, the statistics on LGBTQ-focused sex ed in schools remain low. In a 2015 survey only 12% of the Millennial participants reported that their school’s sex ed curriculum covered same-sex relationships–and that’s not even discussing sexual or gender identity. It becomes clear, then, that it is up to parents and medical professionals to be more educated, to be better allies to LGBTQ kids and youth, and to be a safe space for them. According to the National Center on the Sexual Behavior of Youth “children’s sexual awareness starts in infancy and continues to strengthen throughout preschool and school-age years,” so no matter how young your child is, they know what’s going on with their body and it is your job as a parent to support them.
How can I be an Ally?
Just as it is with any support system, the best way to be an ally is to educate yourself; on LGBTQ history, sex and gender terminology, legal issues, local issues in your city, school issues that may have come up in your child’s school. LGBTQ youth are more likely to be bullied in school, and to search for information on the internet– which often leads them to not credible sources.
- Be a Visible Safe Person: it is important to show your kids you are supportive of the LGBTQ community, and that you are open to conversations about sex and gender. This can be as simple as bringing home a book about queer issues, or a pamphlet from your local Pride Center; you can also initiate conversations about the history, rights, and health of the LGBTQ community. Even a film night is a great way in!
- Support Local Queer Organizations: if there is a Gay-Straight Alliance (GSA) at your child’s school, be an active participant in their efforts for inclusivity, policy, and curriculum changes. If there is a Pride Center where you live, take your kids to family-friendly events. Should a Pride Parade happen in your town or nearby, go the extra mile, or walk the rainbow mile with your kids.
- Provide Reading Materials: just like with any topic, there are age-appropriate books for your child to help them learn more about the LGBTQ community. Visit your local bookstore and ask for the latest publications, and take a look at The Rainbow Collection of the American Psychological Association: https://go.maginationpress.org/rainbow-collection/
- Be a Source of Knowledge: it is impossible to be an encyclopedia for everything your child asks you. But for topics on which misinformation is rampant, is it not important to be a trustworthy source of knowledge? The CDC has an excellent LGBT Health page you can consult as a “crash course,” and they also have a list of regional LGBT Health Services.
Use the Right Words: when your child first becomes interested in their body, or if your toddler or pre-teen asks questions, you can expand the discussion and include appropriate terminology to talk about gender, and talk with them about how pronouns are important outside of their grammar exercises. If your teen is being more direct with their questions, the Gay, Lesbian & Straight Education Network (GLSEN) can help you and them on Inclusive Sexual Health Education, and they can also visit a well-researched and peer-edited page written for teens by teens: https://sexetc.org/
More
By Iris Farrou
19 Jun, 2023
Fatherhood, Mental Health, Parenting, Queer Health, Reproductive health, Sexual health, Women's Health, Young adults & teens
Adolescents, Ally, Bisexual, Gay, Gay-Straight Alliance, Gender Identity, Gender Terminology, Gynecologist, Gynecology, health, Helping my LGBTQ child, Inclusive Sexual Health Education, Intersex, Lesbian, LGBTQ, LGBTQ Youth Support, LGBTQIA+, Neurodivergent, Non-Binary, OBGYN, Pre-Teen, Pride Month, Pronouns, Queer, Sexual Behavior, Teen, Teenagers, Transgender, Youth

A large number of pregnant people experience heartburn during pregnancy, and the logical next step is to see treatment for acid reflux. There is, however, a slight difference between the two terms that may help you differentiate: acid reflux refers to the lower esophageal sphincter (LES) not tightening as it should, which allows the stomach acid to travel up to your esophagus.
Heartburn is a symptom of acid reflux, and it is often experienced as a feeling of burning or pain in your chest. During pregnancy, not only is your body changing to accommodate your baby, pushing all your gastrointestinal organs together and upwards, but your hormone levels also change and affect how you digest food.
How can it be prevented?
First things first, note that more than half of pregnant women report having heartburn in the third trimester. This is more common in women who have been pregnant before, or have experienced heartburn or dealt with acid reflux conditions before pregnancy.
Lifestyle Changes would be the first suggested method of helping you prevent heartburn during your pregnancy. One suggestion is to wear loose clothing as much as possible to avoid further constrictions on your body. You should also avoid lying down within 3 hours after a meal, and if that is not possible, make sure that your head is elevated–which can also help throughout the night as well. Additionally, lying on the left side of the body to sleep or rest has been shown to assist digestion much faster, and thus lessen the feeling of heartburn.
Eating Habits may be another element to address while pregnant. It is advised to eat smaller meals throughout the day instead of 3 big ones so that your body has more time to process the food and digest easily. Eat slowly for the same reasons, and avoid consuming fluids with your meals– instead, consume fluids in between your meals. Sitting up straight when you eat can also be of great help, as well as not eating a big meal late at night/before you sleep. Cravings may not be avoided, but do your best to pace your intake of food and respect the new–perhaps slower and more sensitive–process of your digestive system.
What are safe medications?
Most pregnant people turn to Tums as a safe medication for heartburn during pregnancy. Tums is a typical antacid with a combination of calcium, magnesium, and aluminum salts that help neutralize stomach acid. Pay attention to the dose, however, as a pregnant person should not be taking more than 1000 mg of elemental calcium per day. Additionally, when pregnant, you should avoid long term use of medications that contain magnesium trisilicate.
Your doctor may suggest other medications, specifically a medication that blocks the stomach acid from traveling up to the esophagus and contains sucralfate. A tried and true method is also to avoid citrus foods, spicy foods and caffeine, and increase how much yogurt, milk, and probiotics you take.
https://www.medicalnewstoday.com/articles/what-can-i-take-for-heartburn-while-pregnant-besides-tums#safe-medications
https://my.clevelandclinic.org/health/diseases/12011-heartburn-during-pregnancy#prevention
More
By Iris Farrou
16 Jun, 2023
Diet & Exercise, Health Conditions and Pregnancy, Lifestyle Tips, Nutrition, Pregnancy, Prevention, Queer Health, Women's Health
Acid Reflux During Pregnancy, Besides Tums, Digestion, Digestive Issues, Esophagus, GERD, Health Conditions while Pregnant, Heartburn, How to cure heartburn while pregnant, OTC Medication for Heartburn, Pregnancy, Pregnancy Heartburn Prevention, Preventing stomach issues, Safe Heartburn Medication, Too much calcium, What foods trigger heartburn, What stops heartburn










